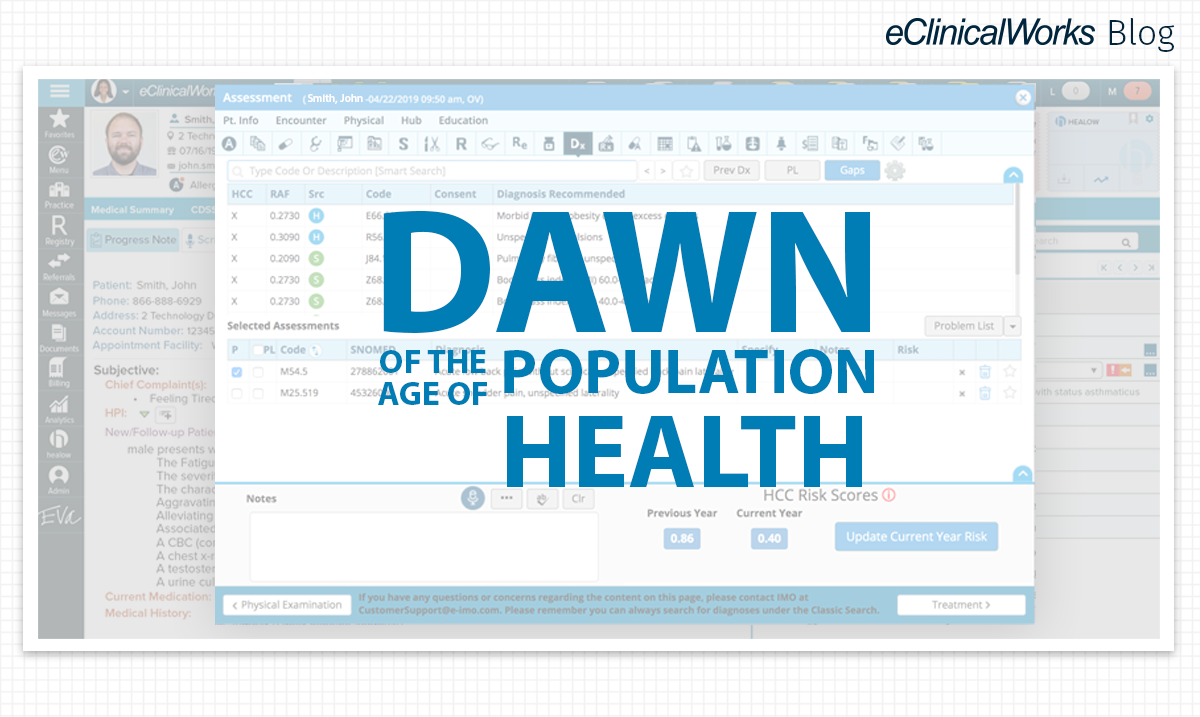
Defying a trend
If you happen to be in the Salt Lake City area and visit any of the 18 locations run by Granger Medical Clinic, you’ll see a lot that looks familiar, including a busy front office and the range of primary and specialty services you’d expect from any growing medical facility.
Look more closely, and you’ll see an organization that’s just a bit different in key ways.
While more and more U.S. doctors are giving up owning their own practices, and joining larger, hospital-owned networks, Granger continues to proudly assert its independence.